It’s easy to forget how important your hips are. They help get you up in the morning, into the shower, and off to see your grandchildren. And when they stop working the way they should, it gets harder to do that normal routine. Every year, many Americans just like you get a hip replaced. In fact, by 2040, experts expect there will be 1.4 million such procedures annually.
If you suffer from hip pain, you’re probably wondering what you can do about it and whether Medicare will pay for it. Here’s what you need to know about hip replacement surgery and how Medicare can help cover it.
Need help navigating your Medicare benefits? Call a licensed insurance agent at (833) 510-0861 to discuss your coverage.
Does Medicare cover hip replacement surgery?
Yes. Medicare can cover hip replacement surgery. In order for Medicare to pay for your surgery, it’s important that your medical records demonstrate nonsurgical treatments such as medicine and physical therapy didn’t work.
Your medical record should also describe in detail the pain you’re having and show the limitations to daily activities that it’s causing. Even the way your doctor and surgery bill for the procedure will influence how Medicare covers everything, so it’s important to provide detailed records whenever possible.
How does Medicare cover your hip replacement surgery?
If you don’t have health insurance, hip replacement surgery could be expensive. Fortunately, Medicare can help you cover the cost. How much help you’ll get from your insurance company depends on which parts of Medicare you have. Here’s a rundown:
- Original Medicare: This includes Medicare Parts A and B. Here’s how the costs break down:
- Part A (hospital insurance): After you cover your $1,556 annual deductible for 2022, Medicare Part A will pay for the hospital stay, including a semiprivate room, meals, general nursing, medications, and other supplies and services.
- Part B (medical insurance): After you cover your $233 annual deductible for 2022, Medicare will typically pay 80% of the approved amount. This will cover most doctor services (including those while you’re in the hospital), physical therapy once you’re out of the hospital, and medical equipment (such as crutches or a walker).You would be responsible for the remaining 20%, unless you have additional coverage.
- Medicare Supplement (aka Medigap): A Medigap plan fills in some of the out-of-pocket costs you might have with Original Medicare. Depending on the plan you choose, that could include your Medicare Part A deductible, your Part B coinsurance and copayments, and more.
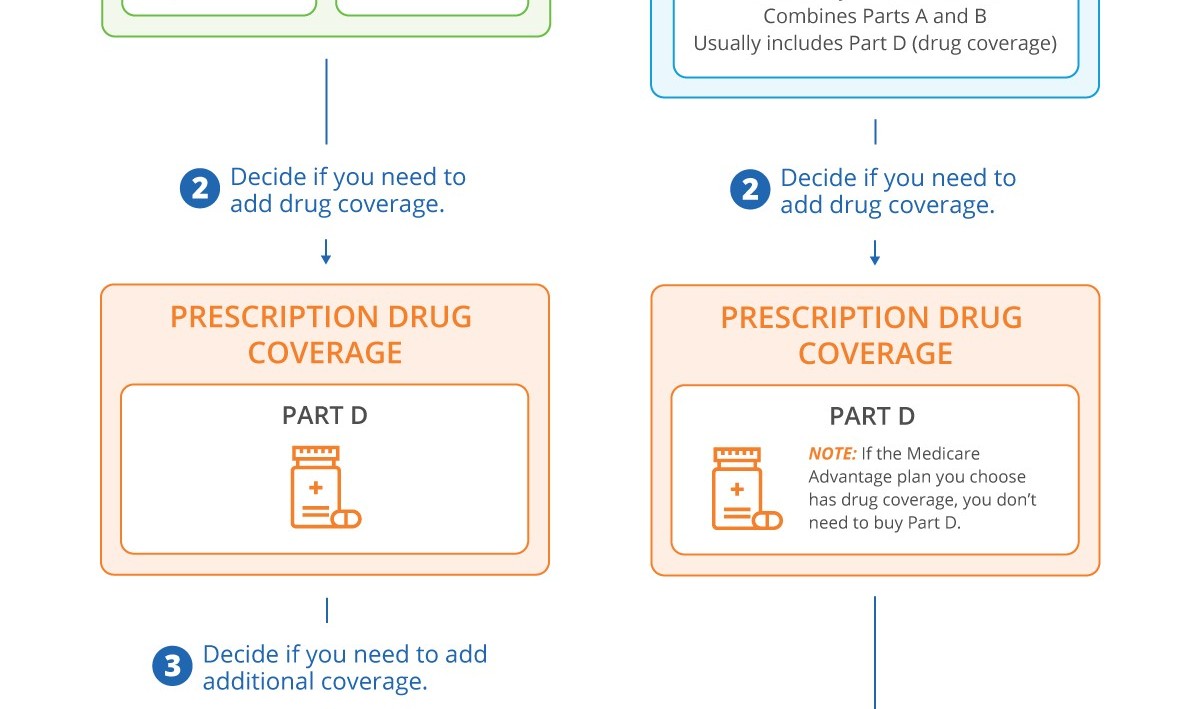
- Medicare Part D (prescription drugs): Medicare Part D, which covers prescription drugs, will cover the medications you may need during recovery, such as pain medications and anti-inflammatory drugs. The specifics of coverage and cost vary by plan.
- Medicare Advantage (aka Medicare Part C): Medicare Advantage (MA) programs are Medicare-approved private alternatives to Original Medicare, meaning they offer benefits that are comparable to Medicare Parts A and B. Medicare Advantage covers everything that Original Medicare does, although what you pay out of pocket varies by plan. Medicare Advantage plans can also include other benefits not available with Original Medicare.
If you’re concerned with the potential cost, you can call a licensed insurance agent at (833) 510-0861. They can help answer questions you might have about Medicare coverage.
Before you schedule your surgery, your doctor might recommend other treatments first
Your hips are two of the largest joints in the body, and they take a lot of wear and tear. The most common way they deteriorate is when the protective tissue between the bones wears down (osteoarthritis). Other ways include autoimmune diseases that harm the joints, such as rheumatoid arthritis, as well as falls and injuries.
Usually, your doctor won’t suggest surgery right away since there are other treatment options. Brian Chalmers, M.D., a bone and joint doctor at the Hospital for Special Surgery in New York City, lists several of the most common and helpful forms of nonsurgical treatment:
- Weight management
- Exercises such as walking, biking, or using an elliptical machine
- Formal physical therapy
- Activity modification
- Over-the-counter (OTC) pain relievers, such as acetaminophen
- OTC and prescription medications, such as ibuprofen, naproxen, and meloxicam
If those treatments don’t work for you, your doctor might then suggest hip replacement surgery
During surgery (aka total hip arthroplasty), a surgeon will replace the damaged parts of your hip with synthetic ones. There are different designs, but they all create a ball-and-socket joint that mimics the structure of the original joint. One part extends from your femur (the long bone in your thigh) and has a ball at the end. The other part creates a socket in your pelvis. A liner in the socket keeps the metal parts from rubbing together.
Depending on your situation, your surgeon might try hip resurfacing as another option. Hip resurfacing is a simpler procedure in which the ball on the femur is capped with a smooth metal covering. But Dr. Chalmers says that this surgery is mostly limited to patients under age 50 who want to stay active doing high-impact activities like running.
What you need to know about recovery
Everybody recovers from surgery differently. But depending on the type of hip replacement surgery you get, you could spend anywhere from 1 to 3 days in the hospital afterward. Or you may get to go home the same day. That’s sometimes referred to as “rapid-recovery hip replacement,” “ambulatory hip replacement,” or “same-day hip replacement.” Whether you spend a night in the hospital or leave the same day, you’ll start physical therapy about 24 hours after your surgery.
“Based on my experience, most patients are able to leave the hospital the same day or within 1 to 2 days of surgery,” says Dr. Chalmers. He adds that patients usually use a walker or cane for the first few weeks, as their hip heals and the pain lessens. Then, after 3 to 6 weeks, they can stop using the walker or cane and start walking longer distances, biking, and doing other low-impact activities.
The good news is that you likely won’t need a second hip replacement surgery for a long time — at least not on the same hip. “The likelihood of a [follow-up] surgery on the first hip replacement with modern implants and techniques is very low at 10 to 20 years, if the [original] operation is done well,” says Dr. Chalmers. “This is even more reason to seek a specialist in hip replacement surgery.”
Bonus tip: consider an ambulatory surgery center
Starting in 2021, total hip replacement surgery joined Medicare’s list of procedures that can be performed at ambulatory surgery centers. Any situation where you have to spend less time in the hospital may benefit not only you and your wallet.
You may also spend less time worrying about the cost of surgery if you have someone to walk you through your Medicare or Medicare Advantage benefits. Call a licensed insurance agent at (833) 510-0861 to talk about your coverage today.