When is the Medicare Annual Enrollment Period?
When is the Medicare Annual Enrollment Period?
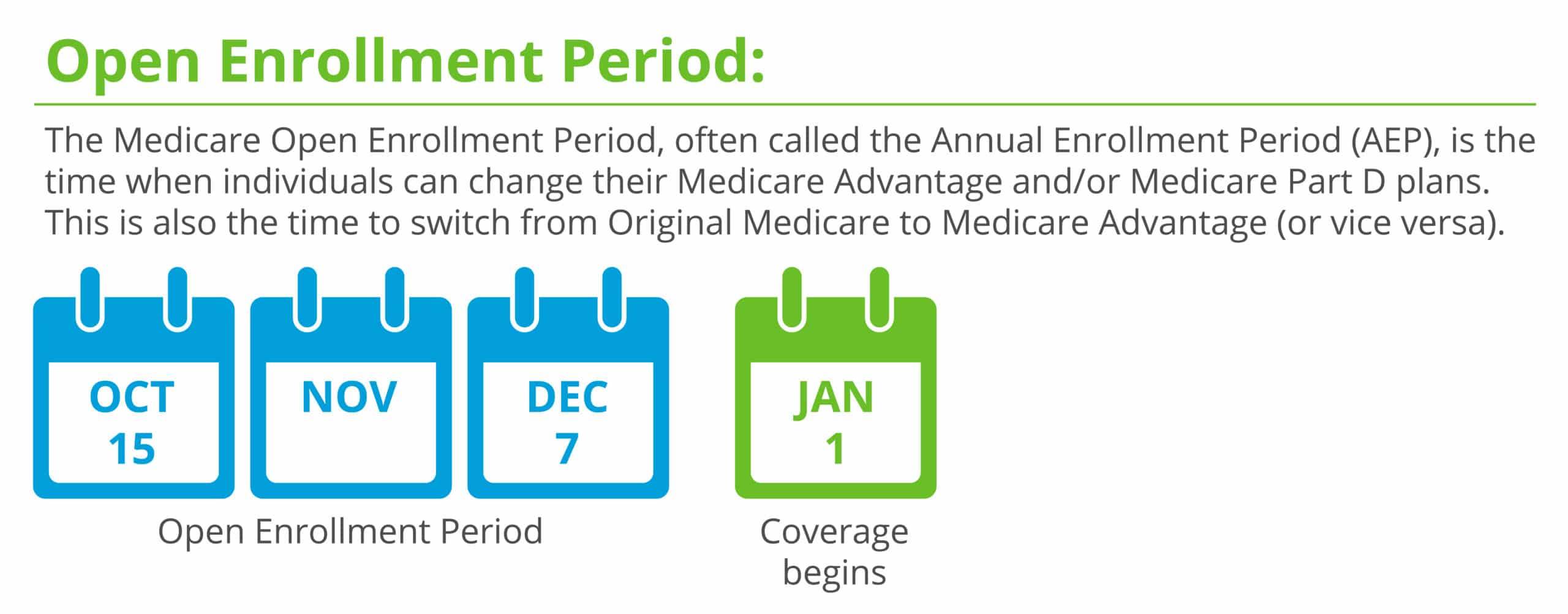
The Medicare Annual Enrollment Period occurs during the fall between October 15 and December 7, 2023.1
When you enroll during this time, your coverage begins January 1, 2024.
When you start to see and hear advertisements for the Medicare Annual Enrollment period on TV, social media, radio, and even old-school mail, plans are trying to get your attention…sometimes in misleading ways.2
So what happens during the Medical Annual Enrollment Period?1
Here’s a simple explanation. You can…
- Enroll in a Medicare plan for the first time during the Medicare Annual Enrollment period if you delayed enrollment during your initial enrollment period.
- Change from Original Medicare (Parts A and B) to Medicare Advantage (MA) and vice versa.
- Add or change a Medicare Part D Prescription Drug Plan to your Original Medicare benefits.
- Switch from one Medicare Advantage Plan or Prescription Drug Plan plan to another.
You’ve got a lot of options to consider during the Medicare Annual Enrollment Period. And we’re here to help you.
In this article, you’ll learn:
- The different names used to describe the Medicare Annual Enrollment Period
- Why you should join a Medicare Advantage or Part D Plan during the enrollment period
- The benefits of reviewing your Medicare coverage during this time
- The difference between the Annual Enrollment Period and Medicare General Enrollment Period
- What to do if you’re getting Medicare for the first time during the enrollment period
- The best time to enroll in Medicare to avoid late-enrollment penalties
Different names for Medicare Annual Enrollment Period
Before we continue, let’s go over some of the different names for the Medicare Annual Enrollment Period. It’s also known as the…
- Medicare Annual Election Period
- Medicare Open Enrollment Period
- Medicare Fall Open Enrollment.
Whenever you see these various names, they are referring to the October 15 to December 7, 2023 Medicare Open Enrollment date. When you enroll during this time, your coverage begins January 1, 2024.
Medicare Annual Enrollment Period |
|||
| The Medicare Annual Enrollment Period, often called the Annual Enrollment Period (AEP), is the time when individuals can change their Medicare Advantage and/or Medicare Part D plans. This is also the time to switch from Original Medicare to Medicare Advantage or vice/versa. | |||
Annual Enrollment Period |
Coverage begins | ||
| October 15, 2023 – December 7, 2023 |
January 1, 2024 |
||
4 things to know about Medicare Advantage & Part D plans for Medicare Annual Enrollment
Wondering if enrolling in a Medicare Advantage plan or Prescription Drug Part D plan during the annual enrollment period makes sense?
Here’s some information that may help…3
- Medicare Advantage (also known as “Part C”) is a type of Medicare health plan offered by a private company that contracts with Medicare. These plans include Part A, Part B, and usually Part D. Plans may offer some extra benefits that Original Medicare doesn’t cover.
There are at least four things to know to help you evaluate your options for a Medicare Advantage or Medicare Part D drug plan during the Medicare Annual Enrollment Period, including:
Here’s some information that may help…3
1. Medicare Advantage includes Original Medicare plus more
Medicare Advantage plans must include Original Medicare Part A and Part B benefits.
Medicare Advantage plans may be a convenient way to get your:
- Part A hospital insurance
- Part B medical insurance
- Other health benefits the plan includes
2. Original Medicare doesn’t cover every medical service
Medical services—such as routine care for dental, vision, and hearing—are not covered under Original Medicare.
- Being able to switch from Original Medicare to Medicare Advantage is one of the main differences between Medicare Annual Enrollment Period.
- Why? You can switch to a Medicare Advantage plan (or change your current plan) during the annual enrollment period.
3. Medicare Advantage plans & out-of-pocket spending
Original Medicare doesn’t have a limit on how much your out-of-pocket costs are for things like coinsurance and copays.
However…
- Medicare Advantage plans have a yearly out-of-pocket limit for covered Part A and Part B medical expenses.
- Medicare Advantage plans pay for all your covered expenses after you’ve reached the plan’s yearly limit.
4. Original Medicare & prescription drug benefits
You don’t get prescription drug coverage automatically when you enroll in Medicare.
To get coverage for your medications, you have a couple of options:4
- You can join a standalone Medicare Part D Prescription Drug Plan (PDP) to add drug benefits to your Original Medicare coverage.
- You can switch from Original Medicare to a Medicare Advantage Prescription Drug Plan during the annual enrollment period, which is the same time as the Medicare Part D Enrollment Period.
Note: Both Medicare Advantage and Medicare Part D Prescription Drug Plans are only available through private insurance companies that contract with Medicare.
4 reasons to review your coverage during the Medicare Annual Enrollment Period
If you’re already enrolled in a Medicare plan, you could sit back and do nothing during the annual enrollment period.
But things change, including things like your health and what a plan covers.
- TIP: Whether you’re currently getting your Medicare benefits through Original Medicare or you’re enrolled in a Medicare Advantage or Medicare Part D drug plan, it’s important that you review your Medicare plan options during the annual enrollment period.
Here are four reasons you may want to re-evaluate your Medicare choices. This gives you an opportunity to make sure:
1. Your coverage meets your current healthcare needs
If your health has changed and you’re not sure if your plan adequately meets your needs, this is a good time to review your coverage.
- You can compare options such as an all-in-one Medicare Advantage plan that includes Original Medicare plus additional health benefits like prescription drug, dental, vision, and hearing coverage.
2. Your current medications are covered
Did you know that drugs on a plan’s formulary can change every year?
Not only that, the price you pay for your medicines can be different from plan to plan, because some plans are able to negotiate higher discounts with certain pharmacies.
Taking a closer look at this during the Medicare Annual Enrollment period could make your prescription medications more affordable.
You can even check to see if you qualify for Extra Help">Extra Help from Medicare to help pay your prescription drug costs.5
3. You can better manage out-of-pocket medical expenses
You can Explore options such as:
- A zero-premium Medicare Advantage plan.
- A Medicare Supplemental plan that offers more flexibility in paying for Medicare’s out-of-pocket expenses, such as deductibles, copayments, and coinsurance.
4. You have access to preferred healthcare providers in your area
This includes your favorite doctors, specialists, healthcare facilities, and pharmacies.
Medicare Annual Enrollment, General Enrollment & Initial Enrollment: What’s the difference?
Unlike the Medicare Annual Enrollment Period, the Medicare General Enrollment Period takes place annually from January 1 to March 31, 2024.
This is the time of year when you can join Original Medicare Parts A and B for the first time if you didn’t sign up for Medicare benefits when you were first eligible during your Initial Enrollment Period.6
An easy way to remember the difference between the Medicare Annual, Initial, and General Enrollment Period is:
- The Annual Enrollment Period is when you can change your existing Medicare coverage.
- The General Enrollment Period is when you can sign up for Medicare Part A and/or Part B for the first time.
- The Initial Enrollment Period is the first time you can sign up for Medicare: 3 months before your 65th birthday, the month of your birthday, and 3 months after your 65th birthday
Getting Medicare for the first time during the General Enrollment Period
If you choose to delay enrollment in Medicare Part A, Part B, or both during your Initial Enrollment Period, you get another chance to enroll during the Medicare General Enrollment Period from January 1 to March 31, 2024.
When you sign up for Medicare during the General Enrollment Period, you may have to pay late-enrollment penalties.7
- The penalty for Medicare Part A applies if you don’t qualify for premium-free Part A benefits and didn’t enroll when you were first eligible.
- If you get Medicare Part B during the General Enrollment Period, you may pay a late-enrollment penalty for the entire time you have Part B.
It’s important to remember that the General Enrollment Period only allows you to enroll in Medicare Parts A and B.
- You can’t switch from Original Medicare to Medicare Advantage or vice versa, or change your Medicare Advantage or Medicare Part D plan during the General Enrollment Period.
Note: The Medicare General Enrollment Period allows individuals to enroll in Parts A and B, but late enrollment penalties may apply and increase premiums. The General Enrollment Period is January 1 to March 31, 2024. If you enroll during this period, your coverage begins July 1, 2024.
General Enrollment Period |
|||
| The General Enrollment Period (GEP) allows individuals to enroll in Parts A and B, but late enrollment penalties may apply and increase your premiums. | |||
General Enrollment Period |
Coverage begins |
||
| January 1, 2024 – March 31, 2024 | July 1, 2024 | ||
Best time to get Medicare to avoid late-enrollment penalties
The best time to sign up for Medicare benefits to avoid paying higher premiums because of late-enrollment penalties is during your Initial Enrollment Period.
- This is the seven-month period surrounding your 65th birthday month.
- But if you or your spouse are still working or you have group health insurance through your current job, you can delay your enrollment.
If this applies to you, you will get a Special Enrollment Period to sign up for Medicare when you or your spouse stops working or your employer-based health coverage ends—whichever happens first.8
Initial Enrollment Period |
||
| The Initial Enrollment Period (IEP) is the first time you can sign up for Medicare. | ||
During the Initial Enrollment Period you can enroll during one of these three periods… |
||
|
3 months before your 65th birthday |
The month of your birthday |
3 months after your 65th birthday |
Need a little help during the Medicare Annual Enrollment Period?
Our licensed insurance agents can help you compare Medicare plans based on your situation. Want to learn more about your options? Give us a call at (800) 827-9990 or find a licensed insurance agent in your area.